Bronchitis
Updated: 2024-07-31
Overview
Bronchitis is an inflammation of the lining of your bronchial tubes. These tubes carry air to and from your lungs. People who have bronchitis often cough up thickened mucus, which can be discolored. Bronchitis may start suddenly and be short term (acute) or start gradually and become long term (chronic).
Acute bronchitis, which often develops from a cold or other respiratory infection, is very common. Also called a chest cold, acute bronchitis usually improves within a week to 10 days without lasting effects, although the cough may linger for weeks.
Chronic bronchitis, a more serious condition, is a constant irritation or inflammation of the lining of the bronchial tubes, often due to smoking. If you have repeated bouts of bronchitis, you may have chronic bronchitis, which requires medical attention. Chronic bronchitis is one of the conditions included in chronic obstructive pulmonary disease (COPD).
Symptoms
If you have acute bronchitis, you may have cold symptoms, such as:
- Cough
- Production of mucus (sputum), which can be clear, white, yellowish-gray or green in color — rarely, it may be streaked with blood
- Sore throat
- Mild headache and body aches
- Slight fever and chills
- Fatigue
- Chest discomfort
- Shortness of breath and wheezing
While these symptoms usually improve in about a week, you may have a nagging cough that lingers for several weeks.
For chronic bronchitis, signs and symptoms may include:
- Cough
- Production of mucus
- Fatigue
- Chest discomfort
- Shortness of breath
Chronic bronchitis is typically defined as a productive cough that lasts at least three months, with bouts that recur for at least two consecutive years. If you have chronic bronchitis, you're likely to have periods when your cough or other symptoms worsen. It's also possible to have an acute infection on top of chronic bronchitis.
When to see a doctor
Contact your doctor or clinic for advice if your cough:
- Is accompanied by a fever higher than 100.4 F (38 C).
- Produces blood.
- Is associated with serious or worsening shortness of breath or wheezing.
- Includes other serious signs and symptoms, for example, you appear pale and lethargic, have a bluish tinge to your lips and nail beds, or have trouble thinking clearly or concentrating.
- Lasts more than three weeks.
Before you go in, your doctor or clinic can give you guidance on how to prepare for your appointment.
Causes
Acute bronchitis is usually caused by viruses, typically the same viruses that cause colds and flu (influenza). Many different viruses — all of which are very contagious — can cause acute bronchitis. Antibiotics don't kill viruses, so this type of medication isn't useful in most cases of bronchitis.
Viruses spread mainly from person to person by droplets produced when an ill person coughs, sneezes or talks and you inhale the droplets. Viruses may also spread through contact with an infected object. This happens when you touch something with the virus on it and then touch your mouth, eyes or nose.
The most common cause of chronic bronchitis is cigarette smoking. Air pollution and dust or toxic gases in the environment or workplace also can contribute to the condition.
Risk factors
Factors that increase your risk of bronchitis include:
- Cigarette smoke. People who smoke or who live with a smoker are at higher risk of both acute bronchitis and chronic bronchitis.
- Low resistance. This may result from another acute illness, such as a cold, or from a chronic condition that compromises your immune system. Older adults, infants and young children have greater vulnerability to infection.
- Exposure to irritants on the job. Your risk of developing bronchitis is greater if you work around certain lung irritants, such as grains or textiles, or are exposed to chemical fumes.
- Gastric reflux. Repeated bouts of severe heartburn can irritate your throat and make you more prone to developing bronchitis.
Complications
Although a single episode of bronchitis usually isn't cause for concern, it can lead to pneumonia in some people. Repeated bouts of bronchitis, however, may mean that you have chronic obstructive pulmonary disease (COPD).
Prevention
To reduce your risk of bronchitis, follow these tips:
- Get an annual flu shot. Many cases of acute bronchitis result from influenza, a virus. Getting a yearly flu vaccine can help protect you from getting the flu. Also ask your doctor or clinic if you need a vaccination that protects against certain types of pneumonia.
- Wash your hands. To reduce your risk of catching a viral infection, wash your hands frequently and get in the habit of using alcohol-based hand sanitizers. Also, avoid touching your eyes, nose and mouth.
- Avoid close contact with people who have a viral infection. Stay away from people who have the flu or another respiratory illness.
- Avoid cigarette smoke. Cigarette smoke increases your risk of chronic bronchitis.
- Wear appropriate face covering. If you have COPD, consider wearing a face mask at work if you're exposed to dust or fumes. Talk to your employer about the appropriate protection. Wearing a face mask when you're going to be among crowds helps reduce exposure to infections.
Diagnosis
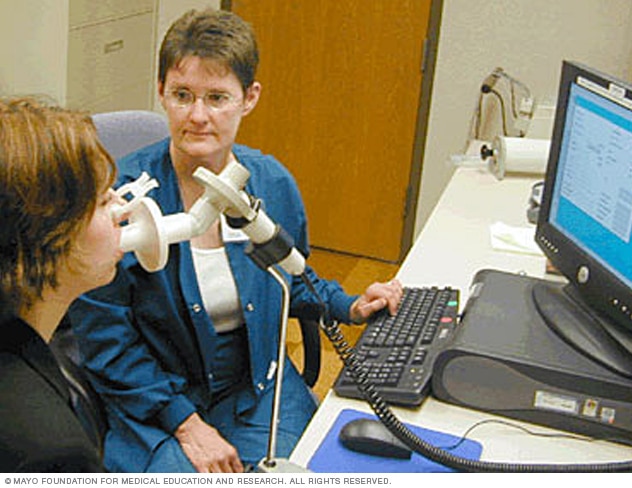
Spirometer
A spirometer is a diagnostic device that measures the amount of air you can breathe in and out and the time it takes you to breathe out completely after you take a deep breath.
During the first few days of illness, it can be difficult to distinguish the signs and symptoms of acute bronchitis from those of a common cold. During the physical exam, your doctor will use a stethoscope to listen closely to your lungs as you breathe.
In some cases, your doctor may suggest the following tests:
- Chest X-ray. A chest X-ray can help determine if you have pneumonia or another condition that may explain your cough. This is especially important if you smoke or have ever smoked.
- Sputum tests. Sputum is the mucus that you cough up from your lungs. It can be tested to see if you have illnesses that could be helped by antibiotics. Sputum can also be tested for signs of allergies.
- Pulmonary function test. During a pulmonary function test, you blow into a device called a spirometer, which measures how much air your lungs can hold and how quickly you can get air out of your lungs. This test checks for signs of asthma, chronic bronchitis or emphysema.
Treatment
Most cases of acute bronchitis get better without treatment, usually within a couple of weeks.
Medications
In some circumstances, your doctor may recommend other medications, including:
- Cough medicine. If your cough keeps you from sleeping, you might try cough suppressants at bedtime.
- Other medications. If you have allergies, asthma or chronic obstructive pulmonary disease (COPD), your doctor may recommend an inhaler and other medications to reduce inflammation and open narrowed passages in your lungs.
- Antibiotics. Because most cases of acute bronchitis are caused by viral infections, antibiotics aren't effective. However, if your doctor suspects that you have a bacterial infection, he or she may prescribe an antibiotic.
Therapies
If you have chronic bronchitis, you may benefit from:
- Pulmonary rehabilitation. This is a breathing exercise program in which a respiratory therapist teaches you how to breathe more easily and increase your ability to be physically active.
- Oxygen therapy. This delivers extra oxygen to help you breathe.
Lifestyle and home remedies
If you have bronchitis, to help you feel better, you may want to try the following self-care measures:
- Get enough rest. Rest and sleep help your body heal.
- Drink plenty of fluids. Staying hydrated can help to thin mucus.
- Avoid lung irritants. Don't smoke. Wear a mask when the air is polluted or if you're exposed to irritants, such as paint or household cleaners with strong fumes.
- Use a humidifier. Warm, moist air helps relieve coughs and loosens mucus in your airways. Be sure to clean the humidifier according to the manufacturer's recommendations to avoid the growth of bacteria and fungi in the water container.
- Consider a face covering in cold air. If cold air makes your cough worse and causes shortness of breath, put on a face mask or cover your mouth and nose with a scarf before you go outside.
Preparing for an appointment
You're likely to start by seeing your family doctor. If you have chronic bronchitis, you may be referred to a doctor who specializes in lung diseases (pulmonologist).
What you can do
Before your appointment, make a list of answers to the following questions:
- Have you recently had a cold or the flu?
- Have you ever had pneumonia?
- Do you have any other medical conditions?
- What medications, vitamins and supplements do you take regularly?
- Are you exposed to lung irritants at your job?
- Do you smoke or are you around tobacco smoke?
If possible, bring a family member or friend to your appointment. Sometimes it can be difficult to remember all the information provided. Someone who accompanies you may remember something that you missed or forgot.
If you've ever seen another physician for your cough, tell your present doctor what tests were done. If possible, bring the reports with you, including results of a chest X-ray, sputum culture and pulmonary function test.
What to expect from your doctor
Your healthcare professional is likely to ask you several questions, such as:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- Do your symptoms affect your sleep or work?
- Does anything improve or worsen your symptoms?
- Does cold air bother you?
- Do you notice that you wheeze sometimes?
- Have you had bronchitis before? Has it ever lasted more than three weeks?
- In between bouts of bronchitis, have you noticed that you're more short of breath than you were a year earlier?
- Do you exercise? Can you climb one flight of stairs without difficulty? Can you walk as fast as you used to?
- Do you smoke? If so, how much and for how long?
- Have you inhaled recreational drugs?
- Have you received the annual flu shot?
- Have you ever been vaccinated against pneumonia? If so, when?